Everything You Need to Know about Diabetic Neuropathy
Diabetic neuropathy is a type of nerve damage that can occur if you have diabetes. High blood sugar (glucose) can injure nerves throughout your body. Diabetic neuropathy most often damages nerves in your legs and feet.
Depending on the affected nerves, symptoms of diabetic neuropathy can range from pain and numbness in your legs and feet to problems with your digestive system, urinary tract, blood vessels and heart. Some people have mild symptoms. But for others, diabetic neuropathy can be quite painful and disabling.
Diabetic neuropathy is a common and serious complication of diabetes. But you can often prevent diabetic neuropathy or slow its progress with proper blood sugar control and a healthy lifestyle.
Types of Neuropathies
A. Peripheral Neuropathy
Peripheral neuropathy is the most common type of diabetic neuropathy. It affects the feet and legs first, followed by the hands and arms. Signs and symptoms of peripheral neuropathy are often worse at night, and may include:
1. Numbness or reduced ability to feel pain or temperature changes
2. Tingling or burning sensation
3. Sharp pains or cramps
4. Increased sensitivity to touch — for some people, even the weight of a bedsheet can be painful
5. Muscle weakness
6. Loss of reflexes, especially in the ankle
7. Loss of balance and coordination
8. Serious foot problems, such as ulcers, infections, and bone and joint pain
B. Autonomic Neuropathy
The autonomic nervous system controls your heart, bladder, stomach, intestines, sex organs and eyes. Diabetes can affect nerves in any of these areas, possibly causing:
1. A lack of awareness that blood sugar levels are low (hypoglycemia unawareness)
2. Bladder problems, including urinary tract infections or urinary retention or incontinence
3. Constipation, uncontrolled diarrhea or both
4. Slow stomach emptying (gastro paresis), causing nausea, vomiting, bloating and loss of appetite
5. Difficulty swallowing
6. Increased or decreased sweating
7. Problems controlling body temperature
8. Changes in the way your eyes adjust from light to dark
9. Increased heart rate at rest
10. Sharp drops in blood pressure after sitting or standing that may cause you to faint or feel lightheaded
11. Erectile dysfunction
12. Vaginal dryness
13. Decreased sexual response
C. Radiculoplexus Neuropathy (diabetic amyotrophy)
Radiculoplexus neuropathy affects nerves in the thighs, hips, buttocks or legs. It’s more common in people with type 2 diabetes and older adults. Other names for this type are diabetic amyotrophy, femoral neuropathy or proximal neuropathy.
Symptoms are usually on one side of the body, but sometimes may spread to the other side. You may have:
1. Severe pain in a hip and thigh or buttock that occurs in a day or more
2. Eventual weak and shrinking thigh muscles
3. Difficulty rising from a sitting position
4. Abdominal swelling, if the abdomen is affected
5. Weight loss
Most people improve at least partially over time, though symptoms may worsen before they get better.
D. Mononeuropathy
Mononeuropathy, or focal neuropathy, is damage to a specific nerve in the face, middle of the body (torso) or leg. It’s most common in older adults. Mononeuropathy often strikes suddenly and can cause severe pain. However, it usually doesn’t cause any long-term problems.
Symptoms usually go away without treatment over a few weeks or months. Your specific signs and symptoms depend on which nerve is involved. You may have pain in the:
1. Shin or foot
2. Lower back or pelvis
3. Front of thigh
4. Chest or abdomen
Mononeuropathy may also cause nerve problems in the eyes and face, leading to:
1. Difficulty focusing
2. Double vision
3. Aching behind one eye
4. Paralysis on one side of your face (Bell’s palsy).
How common is diabetic neuropathy?
Incidences are more common in patients with poor control, overweight, have higher levels of blood fat and blood pressure, and are over the age of 40.
The longer a person has diabetes, the greater the risk of developing neuropathies.
Neuropathy may affect up to 50% of people with diabetes.
Symptoms of neuropathy will often first manifest as numbness or pain in the hands, feet, arms or legs (distal symmetric neuropathy).
However, they may also affect the organs, including the heart and sex organs.
What exactly causes neuropathy amongst people with diabetes?
The exact effect of glucose on the nervous system is still not known.
However, prolonged exposure to higher than normal glucose levels certainly damage the nerves, causing neuropathy.
High levels of triglycerides, a key blood fat which is measured during a cholesterol check, are also associated with the development of nerve damage.
A combination of other causal factors includes:
High blood pressure
Smoking
Alcohol use
Having chronic liver or kidney disease
Vitamin B deficiency
Certain medications, including some anti-cancer drugs, are also associated with bringing on neuropathy.
How is neuropathy diagnosed?
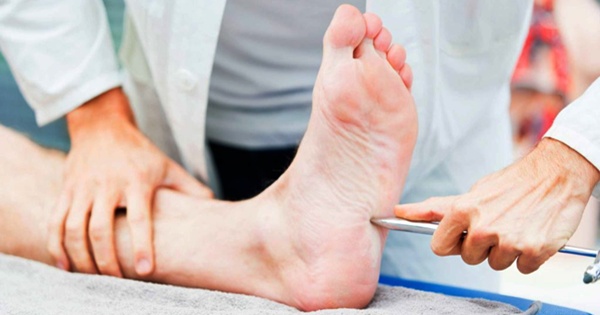
Diagnosis will occur on the basis of your individual symptoms and a physical exam. The doctor may test your blood pressure, heart rate, strength, reflexes and sensitivity. Foot examinations are recommended for all diabetics.
Other tests may be applied, such as:
1. Nerve conduction studies
2. MG (electromyography) and
3. QST (quantitative sensory testing)
Doctors should screen for neuropathy amongst diabetic patients at least once per annum.
How is neuropathy treated?
Diffuse neuropathy is treated by bringing blood glucose levels under control and keeping them well regulated. This can help to prevent problems from this diabetic complication.
Diet, exercise or medication may be adjusted to reach these goals. Exercise can be particularly effective, helping the patient to improve circulation, strengthen muscle and lose weight.
Smoking should be stopped and the amount of alcohol consumed should be reduced. Taking regular care of your feet and skin is essential. Furthermore, the eyes can suffer problems leaving them less sensitive to changes in light.
How do I prevent diabetic neuropathy?
Maintaining consistently normal blood glucose levels is the best way to prevent diabetic neuropathy. Keeping levels stable protects the nerves.
Why is foot care so important?
Peripheral neuropathy makes the foot incredibly vulnerable – hence foot care and general skin care is very important.
Because one of the signs of neuropathy is a loss of feeling, feet should be checked daily for cuts, sores, blisters, bruises and cracked or dry skin. If you notice anything unusual, get to your doctor as soon as possible.
Featured image courtesy: Reader’s Digest.
Sources:
2. myoclonic.org
3. National institute of Diabetes and Digestive and Kidney Diseases.
Disclaimer: The views expressed here are solely of the author. My India My Glory does not assume any responsibility for the validity or information shared in this article by the author.
Dr. Das Partha Sakha
Latest posts by Dr. Das Partha Sakha (see all)
- Everything You Need to Know about Hypothyroidism - July 27, 2024
- What is a Healthy Balanced Diet for Diabetes? - July 27, 2024
- Top 10 Diabetic Super Foods - July 27, 2024